Fatty liver disease, or hepatic steatosis, is a condition where fat accumulates in the liver, affecting its ability to function properly. While it often starts silently and without symptoms, it can progress to serious liver damage—including cirrhosis and liver failure—if left untreated. With the rise in lifestyle-related conditions like obesity, insulin resistance, and type 2 diabetes, nonalcoholic fatty liver disease (NAFLD) has become alarmingly common.
According to research, up to 25–30% of adults in the U.S. and Europe may have NAFLD, often without even knowing it.
Let’s explore the top three signs of fatty liver disease that you should never ignore, and understand what’s happening inside your body when these symptoms appear.
⚠️ 1. Extreme, Persistent Fatigue
Feeling tired occasionally is normal—but if you’re constantly drained, even after a full night’s sleep or a restful weekend, your liver may be the culprit.
🧠 Why does fatty liver cause fatigue?
The liver is a powerhouse organ responsible for metabolizing nutrients, filtering toxins, and regulating blood sugar. When it’s overburdened by fat accumulation:
- It becomes inflamed and sluggish.
- Toxin removal slows down.
- Brain function and energy regulation are disrupted.
This leads to persistent fatigue, poor concentration, irritability, and sometimes even low mood or depression. Many people describe it as a sense of heaviness or exhaustion that feels like “trekking uphill every day.”
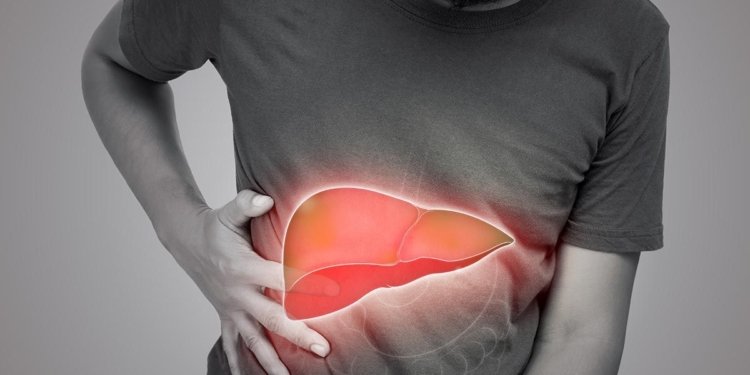
⚠️ 2. Pain or Discomfort in the Upper Right Abdomen
Fatty liver may cause a dull ache, pressure, or even sharp pain just under the right rib cage—where your liver is located.
🧬 The science behind the pain:
- The liver has no pain receptors itself, but it’s enclosed in a membrane called Glisson’s capsule, which does.
- When fat builds up and causes liver enlargement, this capsule gets stretched, leading to discomfort.
This symptom is often subtle at first but can become persistent and even disturb sleep. It may come and go or be mistaken for gas, gallbladder issues, or even musculoskeletal pain.
📝 Note: Not everyone with fatty liver feels pain, but if you’re at risk and experience this type of discomfort, it’s time for a liver check.
⚠️ 3. The Most Dangerous Symptom: No Symptoms at All
Perhaps the most dangerous aspect of fatty liver is its “silent” nature. Many people with the condition have no symptoms for years, until it’s discovered incidentally during:
- Routine blood tests (elevated liver enzymes: ALT, AST)
- Ultrasounds or scans for unrelated issues
- Advanced stages like fibrosis or cirrhosis
That’s why early screening and awareness are key, especially if you fall into a high-risk category.
🧬 Understanding the Stages of Fatty Liver Disease
Fatty liver disease progresses through four stages:
- Simple Fatty Liver (steatosis): Fat is present but no inflammation. Usually harmless if addressed early.
- Steatohepatitis (NASH or ASH): Fat + inflammation. This stage can progress silently.
- Fibrosis: Persistent inflammation leads to scar tissue formation.
- Cirrhosis: Extensive scarring causes irreversible liver damage and increases risk of liver failure or liver cancer.
✅ Causes and Risk Factors
🔹 Non-Alcoholic Fatty Liver Disease (NAFLD) risk factors:
- Obesity or belly fat
- Type 2 diabetes
- High cholesterol or triglycerides
- Metabolic syndrome
- Poor diet and sedentary lifestyle
- Polycystic ovary syndrome (PCOS)
- Obstructive sleep apnea
- Certain medications (methotrexate, tamoxifen)
🔹 Alcoholic Fatty Liver Disease (AFLD) risk factors:
- Chronic alcohol use (especially >14 drinks/week for men or >7 drinks/week for women)
- Genetics
- Smoking
- Co-existing viral infections (e.g., Hepatitis C)
🧪 How Is Fatty Liver Diagnosed?
If you suspect fatty liver, your doctor may recommend:
- Liver function tests (ALT, AST)
- Ultrasound, CT scan, or MRI
- FibroScan to measure liver stiffness
- Liver biopsy (in more serious or uncertain cases)
💊 Is It Reversible? Yes—With Timely Action!
There’s no approved medication yet for NAFLD or NASH, but lifestyle changes can dramatically improve or even reverse the condition.
🥗 Lifestyle Tips:
- Lose 5–10% of your body weight gradually
- Eat a high-fiber, low-fat, low-sugar diet
- Cut back on saturated and trans fats
- Avoid alcohol (especially if diagnosed)
- Exercise regularly (30 minutes most days)
- Avoid unnecessary medications or supplements that burden the liver
- Consider vitamin E (only under medical guidance)
🛡️ Prevention Is Better Than Cure
To lower your risk of fatty liver or prevent progression:
- Maintain a healthy weight
- Monitor blood sugar and cholesterol
- Eat balanced, antioxidant-rich meals
- Stay hydrated and avoid processed foods
- Get regular liver checkups if you’re at risk
🧾 Final Thoughts
Fatty liver disease doesn’t always shout—it whispers. By the time symptoms like fatigue or abdominal pain arise, some liver damage may already be underway. However, with early detection and healthy lifestyle choices, this condition is largely reversible.
👨⚕️ If you’re feeling unusually tired, experiencing unexplained abdominal discomfort, or have risk factors like obesity or diabetes—get your liver checked today.
Your liver works hard for you. It’s time to return the favor.